At the Doctor’s Office
Regular readers of this blog will remember the article last year in which I wrote about my overnight stay at the sleep lab at St. Joseph’s Health Centre. I got the results a while back, but it was only a couple of weeks ago that I saw my doctor about the results. (I’ll admit it. When it comes to matters medical, I’ve tended to put things off.)
“At one point, you were registering thirty-three apneas an hour,” said my doctor, pointing to my sleep lab results. “When that happens, you make this sound,” after which he made a sound at the back of this throat that sounded like a combination of snoring and choking.
“That…sounds bad.”
“That’s actually classified as severe,” he said.
“I thought that only happened if you were really overweight,” I said, “Say, in the weight class where you have to book two seats on a plane.”
“Well, losing weight can reduce apneas, but even if you’re at your ideal weight, you can still have it.”

One gag-a-riffic examination with a tongue depressor later, he said “You’ve got a narrow airway. That’s a big factor with sleep apnea.”
“So,” I said, “what are my options?” I was already dreading the answers.
“Weight loss will lessen your sleep apnea, but it won’t completely fix it.”
“I could stand to work out a little more,” I said, patting my gut.
“There are mouthpieces you can get, but they’re not always effective. There’s also surgery, which also isn’t effective — it’s basically scraping the inside of your airway, and it can actually make the other methods less effective.”
I already knew where this conversation was going.
“The most effective solution for you is…”
“CPAP?” I asked.
“CPAP,” he replied.
I must have grimaced at the thought of spending the remainder of my sleeping life hooked to a machine, because he said “You’ll be surprised at the difference it makes.”
CPAP
CPAP (pronounced “SEE-pap”) is an acronym for “Continuous Positive Airway Pressure” and is used to refer to the machine used by the man pictured below:

Sleep apnea is caused by the upper airway being closed off when the muscles relax during sleep. This cutting off the of the airway leads to a loss of oxygen, which triggers an automatic fight-or-flight response from the cardiovascular system and brain, which causes a waking response. This sort of thing, repeated over and over again, messes with your sleep and puts undue strain on the heart.
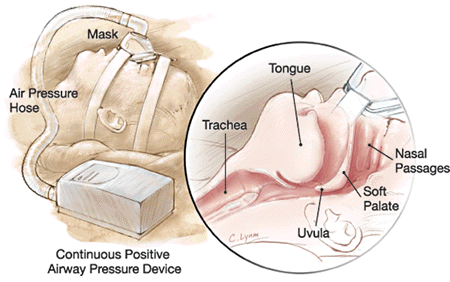
A CPAP machine provides pressurized air to the nose, which inflates the airway, keeping it continuously open. The end result is unobstructed breathing, which in turn eliminates sleep apnea and as an added bonus eliminates snoring.
The downside? You spend all night in something that looks like a gimp mask. (I’m aware that there are a number of people out there who do not see this as a downside.)
CPAP Shopping
With a prescription and list of CPAP stores given to me by my doctor, I set out to do some CPAP machine shopping.
Lesson #1 of CPAP shopping: it’s not like shopping for a computer, DVD player or any other household or office appliance. You have to make an appointment since it takes about an hour and a half to get fitted, and here in Accordion City, it’s pretty much a Monday-to-Friday business.
The guy at the CPAP store was pretty nice and showed me a number of CPAP machines and masks, explaining the differences between them. As I looked over the different models, I thought that CPAP shopping might be a good way for techies like myself to understand what non-techies go through when shopping for computers and electronics.
I decided that the best strategy would be to go with the machine and mask combination that was the most comfortable. If it didn’t feel good, I figured, I wouldn’t use it regularly.
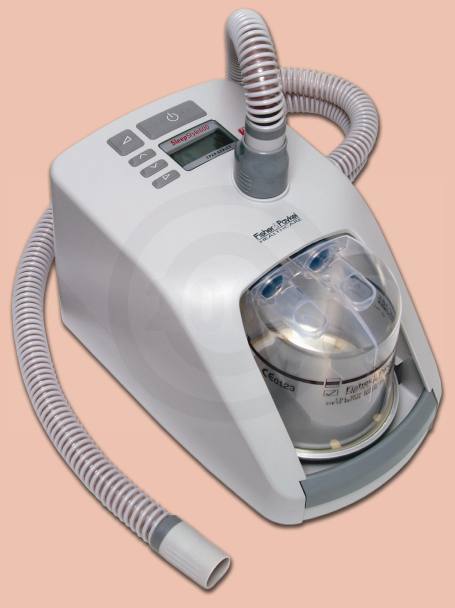
In the end, I chose the machine shown above: a Fisher and Paykel SleepStyle 604. It was squarely in the middle of price range and had the most comfortable-sounding features, including the best humidifier unit and a tube with a heated coil around it to prevent condensation. The more expensive unit, the ResMed (it’s the blue-and-white unit shown in the photo above with the man in bed) was smaller and looked nicer, but the store’s customers have reported that its humidifier wasn’t all that good.
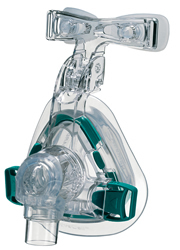
Although the unit came with a mask, it was recommended that I pick out a mask that was a little more comfortable. The up-the-nose mask (like the one in the photo with the man in bed) obstructs your vision the least, but it wasn’t comfortable at all. I ended up going with the ResMed Mirage Activa pictured above because it felt flexible and comfortable. Although you can’t tell from this photo, the mask goes over the nose, not the mouth.
“Now for the fun part,” said the guy at the CPAP store. “Let’s hook you up.”
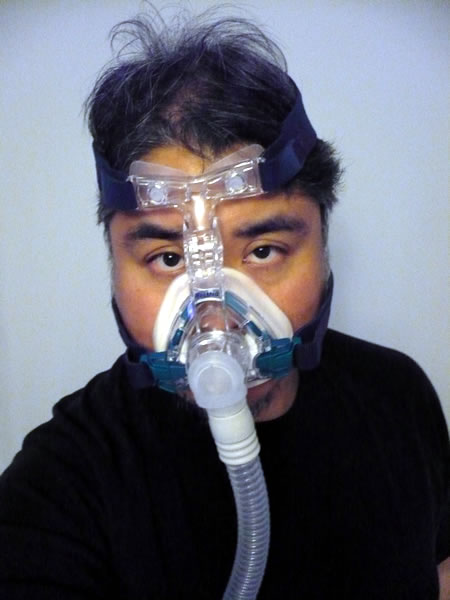
Bring out the gimp!
I was put in a reclining chair and strapped into my CPAP machine and mask. I felt like a muzzled dog.
“This will feel weird at first,” he said and the turned the machine on. A rush of air filled the mask. “Now breathe normally through your nose.”
I did, and despite the increased air pressure, it didn’t feel too weird.
“Now try breathing through your mouth or talking.”
As soon as I opened my mouth, it started venting a rush of air. It didn’t hurt, but it made me instinctively close my mouth.
“Yeah, that’s the pressurized air from the machine. When your mouth is closed, the air goes into your airway and holds it open. With your mouth open, it goes out your mouth and bypasses the airway. When that happens, your CPAP isn’t effective. So don’t open your mouth.”
“Not much chance of that,” I said. I should’ve just said “Okay,” because talking with the machine on is uncomfortable.
I walked out of the store with the machine and mask, carrying cases for both and a service plan (they service the machine, and also check its “odometer” to see that you’ve actually been using it). The total cost was about $1400, half of which will be covered by Ontario’s healthcare plan. I covered the other half on my credit card; the health coverage from work will reimburse me for that.
Back to the Sleep Lab
The next step: titration (pronounced “tie-TRAY-tion”, not “tit ration”). That’s the process where the appropriate amount of air pressure for the CPAP is determined, which requires someone to monitor you while you sleep.
This meant a return to the, the St. Joseph’s Health Centre Sleep Lab. Here’s the bed:
…and here’s the camera over the bed:

Here’s an interesting thing about the camera: the purple lights you see in the photo aren’t visible to the naked eye. They are visible through the LCD viewfinder of my digital camera. I assume that they’re ultraviolet and that the sensor in digital cameras has a wider range than human eyes.
As with my last visit to the sleep lab, I got wired up with a lot of sensors:
- On my forehead
- Behind by ears
- On my head (which meant that I had hair full of electroconductive goop)
- On my neck (a piezoelectric sensor to detect snoring)
- A band across my chest
- A band across my stomach
- On my lower legs (to detect leg twitching)
- On my right index finger (heartbeat monitor)
Here’s the box into which one end of the probes went:

…and here’s where the other end of the probes went:

Unlike my last visit, I had a little more trouble falling asleep. The throat mic was scratching my neck, and it took me a little time to get used to wearing a CPAP mask, air pressure and all. Near the beginning, my mouth would relax a couple of times, causing it to open slightly, which made me spit slightly in a zerbert-like way, which woke me up. I eventually got used to all these new sensations and drifted off…
Awake. Really, Really Awake.
…to be woken up at 6:30 a.m.. Under normal circumstances, a 6:30 a.m. wake-up after 6 hours of sleep would leave me groggy, but I felt quite alert. Under the circumstances, this was a very unusual feeling. I felt very well rested, as if I’d had 8 or 9 hours’ sleep.
I went home, showered and got dressed and went to work. I didn’t have my middle-of-the-afternoon lull where I’d need to get some caffeine or go for a walk to wake myself up and stayed very sharp through the whole day. “It’s like Flowers for Algernon! Well, the first part, anyway,” I said.
That night, I used the CPAP for the first time at home, and Wendy was very pleased at the silence. Aside from the very quiet sound of the CPAP (a gentle whoosh, much quieter than the fan on most computers) the room was silent. No snoring. If she can get used to looking over at my side of the bed and seeing me all “hosed up” — she calls me “The Hosebeast” now — we’ll be golden.
(Wendy would also like it if I would refrain from re-enacting Denis Hopper’s “nitrous oxide” scenes from Blue Velvet with my CPAP mask [not safe for work]. But I have to be me!)
52 replies on “CPAP (or: Snorkeling While I Sleep)”
My 2 cents: it is scary to look at Joey when he has the mask on; it echoes the ICU of which we saw far too much with his dad. But the absence of choking sounds is a huge, huge relief. I just have to be a brave little camper.
What a great summary of your experience and explanation of benefits. I really think it’s probably the answer I’ve been looking for, the only problem is the $1400 portion of that answer and wearing a mask. Never been much of a person that likes stuff on their face. We’ll see.
@bnpositive: I’m glad that this article had useful info for you. Feel free to ask more questions!
My wife has had a machine for half a year or so.
– its rather scary to hear it start pushing air when you are awake and the person beside you is apnea-ing(?)
– you might want to invest in a nose and mouth mask as you cant wear the nose mask when you have a cold (and therefore cant breathe through your nose). her having a simple cold these days freaks me out as we dont (yet) have one that covers the mouth as well
– her dr mentioned there is a pretty decent correlation between weight loss and and starting to wear the mask since (as you discovered) you suddenly have ‘normal’ energy levels
-adam
So…it’s like having a set of bellows pushing air into your lungs…for sleeping?
Awesome.
@Andrew: Well, if you consider only the “exhale” action of bellows, then yes. The additional air pressure (7 cm/water in my case) and the feeling of an inflated airway take a little getting used to.
@Adam Goucher: Thanks for the info!
I’m looking forward to being a little more productive at work as well as with my recreational hacking.
My dad uses a CPAP machine, and he has some suggestions for when you travel… always take it as a carryon (it’s fragile) and be prepared to find the distilled water you need for it when you get to where you’re going, unless you packed a bottle in your checked luggage. We spent two hours trying to find an open store that sold distilled water when we were overseas!
Also, be fastidious about cleaning it! 🙂
Thanks for sharing your experiences so far.
I sleep on my side, and usually turn to the other side at least once during the night.
I may need a similar device, and one thing that concerns me is will I still be able to do that? That is, is the hose long and flexible enough to sleep on your side, facing the inside of the bed?
Welcome to the club! I’ve been on a CPAP machine for a year and a half now. My apena was pretty bad, I think my readings were about double yours. Thankfully the machine did the trick and sleeping with and without it is like night and day.
Joey, I’m so glad that it’s working for you — and so fast! I’m still struggling, as I habitually have nasal congestion after 75 minutes, so I can never stay asleep throughout the night. Your post has finally prompted me to see about getting a full-face mask.
Marriages have been known to suffer because of all that snoring, so putting up with a little bit of Frank Booth seems a small price to pay. Not to mention the enormous health risks if it’s not treated.
Adam: Here’s an article that helps explain the relation between sleep and weight loss: http://www.webmd.com/sleep-disorders/guide/lose-weight-while-sleeping
Thanks for posting this. Every little bit of awareness can help save lives.
@mike: You asked:
I think so, but I’ll double-check when I go home. I’ll take a photo and post it here.
@Allie: The guy at the CPAP shop also told me that I should carry it on the plane rather than checking it in.
As for distilled water, I figure I’ll have to carry some when either flying outside North America or landing late at night in an unfamiliar locale.
And yes, I’m keeping it clean!
Hook up the mask to your accordion when you’re playing it, Joey, that would make quite the sight on Halloween 🙂
Glad to hear you’re getting more sleep though.
Bonne nuit!
Dude, when did your hair go grey?????
Oh, and I have a(nother) question… why does OHIP only cover half the price?
Glad you got treatment I put mine off for years. I could kick myself now for waiting so long. I started with a mask similar to yours and settled on the Resmed Mirage II in the second picture. The difference has been AMAZING to say the least.
[…] « CPAP (or: Snorkeling While I Sleep) […]
Didn’t Homer have one of these at one time? 🙂
Also, I noticed that the CPAP Society and Twitter have something in common. I think this might be a little more than a coincidence, no?
does it come with matching flippers?
Hey Joey. My father went through this and it made a huge difference in his life.
There are some areas I’d like to talk about next time I see you, though.
… to do with sleep clinic knuckleheads.
Carson
Good for you Joey. I often wonder if my sleep problems are caused by that as well. Oddly enough I started sleeping with earplugs and I’m sleeping better. Hmm.
I went through the whole shebang last octoberish – I actually went with the one in the picture, because I wear glasses. It doesn’t bother me.
A couple of things that my doctor told me: Expect to need a pressure adjustment after a few months. Bodies are stupid, and apparently they can get used to the amount of pressure, and need it shifted upwards.
Two: The grey hair? Caused by sleep apnea. Seriously. I’m in my mid twenties and going very badly grey because of it (my numbers are also six times yours.)
Three: Ohip doesn’t really cover half the price. They cover about 75% of a standard base machine price, with absolutely no extras. Mine was a bit above the base, because I wanted the nasal pillow and not a full face mask.
Four: Wendy, just think of it this way: now you get to fully develop all your best darth vader fantasies.
[…] wrote a big post yesterday about his CPAP. I made a short comment on the post but of course I have more to say. When do I […]
Holy moley batman! Still, how awesome is Health Canada! And now you sleep and have a machine that everyone secretly envies. Well done.
[…] received a lot of email resulting from my CPAP article. Many emails asked me about the costs of a CPAP machine. I’m only too happy to provide a […]
I went thru the sleep lab experience last year. Rather to my surprise, since my wife tells me I have the snoring and broken breathing patterns common to sleep apnea, the results showed no signs of apnea.
I must admit to a bit of relief at not having to cyborgize myself every night, but it would be even nicer to not have major sleepy-atacks during the day. (The main reason seems to be an inability to get more than about six hours sleep per night. I use Breathe Right strips on my nose nightly, which make six hours sleep feel like seven, but I still have to take Provigil to get thru most days. This is one of the major reasons I’m retiring from the Postal Service in a few months and looking for a new career that will ONLY be 40 hours a week; the hours currently eaten up by overtime and involuntarily-cancelled days off will be better spent trying to get a full eight hours each night.)
Thanks for sharing your experience! I am a Nurse Practitioner Student and am teaching a lecture to my fellow soon-to-be NP’s on sleep apnea. Having the perspective of the patient is wonderful and so helpful in building better practitioners! May I use the pictures you’ve posted of what CPAP mask looks like on and your comments about it in my lecture next week?
Thanks again for sharing your experience!
@Kathy Fry: Feel free to use any part of this article, photos and text, for your lecture!
I went through this exact same experience, being diagnosed with moderate sleep apnea, (stop breathing 26 times an hour.) and it’s great to read that others are going through the same experiences. I have been using mune for about a week now and notice a HUGE difference. Way more energy and memory. I have the nasal pillows and they are uncomfortable. To those of you contemplating the pros and cons, it’s worth it. The quality of life increase is amazing. I still can’t bring myself to wear the mask while entertaining ladies though. Thanks accordian man!
[…] had to stop at a grocery store to pick up some distilled water (grumble grumble CPAP grumble). Luckily, we had a GPS, and it led us to […]
anonymous here.
thank you for posting this, helped me and countless others. wish i had this info BEFORE i was diagnosed some years ago
[…] a good chat about all sorts of topics: pain, sleep lab sessions (his were far more interesting than mine), Mormon philosophy and musical instruments. His recent trips to “N’awlins” have […]
I just got my CPAP, but I haven’t found a site yet where people realize you can carry distilled water on a plane in larger quantities than the 3 ounce TSA limit for liquids. On the TSA website,http://www.tsa.gov/311/311-carry-ons.shtm they say that liquids in quantities larger than 3 ounces can be brought as carry-ons if they are for medical purposes. My doctor gave me a generic letter for my CPAP machine just in case and added a line at my request that says I need to carry up to 32 ounces of distilled water with the machine. As a frequent traveler this avoids the trouble of searching for a store that sells distilled water when I travel.
Hey Joey,
Been lurking your site for some time, quite informative and entertaining. Yet I randomly came across your blog again while searching for somewhere to DIY fix my CPAP machine. I didn’t know you wrote this article… now I’m glad I found it because people ask me for an explanation all the time and this is pretty much it. Unfortunately I’ve lost my insurance before my machine broke. I and am without my machine and it’s a total nightmare. People have no idea the difference in our lives it makes to be able to sleep properly…
Anyway thank you for the fantastic descriptive article, now I know where to send people that want to know more 🙂
I use a CPAP.
Best thing I got from your blog: made me sure I need to get settings adjusted on mine, has been several years since I acquired, and was not asked to go back to lab to get settings … I think. That sounds so unlikely! In any case, I don’t think mine is keeping the airways open. I would so love to feel I’d had a good night’s sleep!
Doesn’t need water input, though would be nice in this dry climate.
No hassles with planes, the screeners seem to recognize it easily, so there must be a lot of them/us traveling.
The hose is good for turning, has a pivot at the machine end, and at nose mask hose can turn 360′ [that’s a “degree” by someone who….]
Ok, I was just diagnosed, got the news today. I have episodes 37 x’s an hour that last up to 20 seconds each. I guess thats pretty bad? Anyway, I go to a class to learn more and get my Machine next Thursday. I hope it works really good because I am SO TIRED all the time! I have headaches and no energy. I am naturally a social person and my work requires quick thinking and a lot of exposere to the public. For the past 4 -5 years I feel like I’m in a fog and I don’t enjoy the things I used to. In fact I don’t enjoy much of anything. How depressing! I can’t wait to be “born again”! A mask at night for my life back will be a GODSEND! I really hope it work and I can get used to it. I love the Darth Vader comments. I’m sure my husband, and every other living thing in the house will prefere the sound of air over my Gag, Snort and Gasping! Scares my husband. I am also looking forward to being able to watch a TV program all the way to the end without being kicked or strongly nudged to stop the roaring.
Thank you for posting your experience. I’m going for my first sleep study tonight and didn’t know what to expect. Now I do. I also now know what to expect when they tell me I need the cpap machine. I’m fairly certain that’s where I’m headed. Now if I can only convince my wife that she should go get tested too. Then we’d only have to listen to the dog snore.
I’ll let y’all know how it goes.
Cheers.
I was diagnosed with sleep apnea after seeing my ophthalmologist, who detected cupping (nerve damage) on my right optic nerve. We did a visual field test and discovered I have a blind spot as a result of the damage..She suspected glaucoma. but I had normal eye pressure. Before going with eye drops for the rest of my life, I saw a neurologist who suggested I get a sleep study done. Sleep apnea causes wild blood pressure swings all night, which we suspect caused the optic nerve damage.
Long story short, I’m getting a CPAP machine soon and we hope that will stop the progression of the nerve damage. It was helpful to see what the machine looked like (I was imagining some gigantic air compressor thing like I got in my garage). Thanks man.
I recently started using a cpap machine to treat apnea, and found your blog while doing a litle research on my machine.
I enjoyed your descriptions of the sleep lab experience, and the “gimp” mask enormously.
Thank you for the valuable information and the positive way it was presented.
Regards,
Aldo
I was told I did not have sleep apnea, but i do suffer from it every night for years. I wake up with my body numb and have to initiate breathing- I feel like I have been under water for minutes. My memory is terrible and I think itis because of not getting oxygen at night. I have been crying reading your blog because I wish I could be diagnosed. The people at my sleep center did not believe I had apnea; they said, does anyone hear you snore? and I said, i sleep alone. They said, well then , how is it that you can ‘know’ that you have sleep apnea?”. I got so mad at them and I am still mad at them after all these years. I still suffer every night. They don’t understand that I wake up in order to breathe. They told me that “if you know you have sleep apnea, then you don’t have it, because you wouldn’t know it, because you’d be sleeping” . They were such jerks but the receptionist was really nice. I called her and cried about not being diagnosed. I had no insurance so I couldn’t afford to pay 1,000$ dollars for the sleep study. I wish i lived in Canada! I’m in U.S. Of Bad Health A. Please tell me what you think, as I am desperate and feel I can’t trust doctors. I also have a deviated septum in my nose. Insurance here in the US for women is starting at 300 a month, and that doesn’t cover sleep studies, of course.
Enjoyed reading your post! I’m 30, exercise plenty, but have sleep apnea, similar experience to yours. I get about 30 disturbances a night according to my study. Was thinking about removing tonsils, but definitely getting a CPAP now!
could I have permission to use your images for some e-learning we are putting together for nurses to learn about copd and slepp apnoea. we are a not for profit charity in the UK.
ChrisX
Thank you for an informative post. I loved the comments from other users of CPAP. I go tonight to the lab to try the machine. I apparently have 18 episodes/hr.and 55 episodes when I am in REM stage. Not sure why this is different. Any answers? I appreciate all the input since I was starting to chalk this up to a new “business/money maker”. I guess it is worth the try. I would love to wake up refreshed and functioning normally for a change. I’m not sure what that would be like, but it must be better than trying to function with a class of elementary kids all day when I feel so exhausted! I’ll let you know how it goes.
Karen: Good luck! I was stunned at the “before/after” difference with CPAP, and I hope your experience is the same!
@Joey deVilla thank you for this wonderful article and all the information
I am new to the world of sleep apnea and cpap but I can see that the biggest thing especially for me is getting the right mask. I am using my mask in combination with a nasal pillow.
[…] what I saw just before I turned out the lights. The funny apparatus with the hose is my CPAP. Although it’s a pain in the ass to bring along on trips, I still function much better when I […]
[…] do I explain the CPAP to a girl who “sleeps […]
I used my CPAP machine for the first time last night. It wasn’t bad at all with the nose mask and the humidifier kept my mouth not dry and I could swallow without feeling that my tongue has turned into a sandy thing. I slept without hearing my husband’s snore and I didn’t snore at all. It was a dreamless sleep and I feel really good this morning.
Good story Joey!
I use my bi-pap since 2002 and I love it.
Before that I was more dead then alive most of the time.
I am a regular contributer of a Fb page about Sleepapnea here in Holland (Netherlands) where people can post there experiences and help eacheother with questions. Or get advice and so on.
Harry
[…] Nearly eight years ago, I started using a CPAP (pronounced “SEE-pap”) machine while sl… I have sleep apnea, which I wrote about in April 2008: […]
[…] Nearly eight years ago, I started using a CPAP (pronounced “SEE-pap”) machine while sl… I have sleep apnea, which I wrote about in April 2008: […]
[…] I’ve been a CPAP user for about 15 years, and a fan of The Clash for far longer. […]